Diseases of the musculoskeletal system in almost all cases are accompanied by dysfunction of its organs, which causes a lot of discomfort to the patient.
An important symptom of pathologies of the musculoskeletal framework is pain. Joint injuries are especially unpleasant.
The hip is the largest of them. Pain in case of his defeat can be localized around him and give it to various anatomical structures: to the organs of the small pelvis, lower back or thigh.
General classification of causes
The etiology of hip pain is varied.
In medicine, the following causes of arthralgia are conditionally distinguished:
- Inflammatory and infectious processes within the joint and its surrounding tissues.
- Degenerative diseases of the musculoskeletal system.
- injuries.
- Bone and soft tissue neoplasms.
There are other specific causes of arthralgia:
- Piriformis syndrome. Associated with its prolonged spasm.
- Femoral head necrosis (GBC). Most of the time it is a complication of another pathology of TBS.
- Legg-Calvé-Perthes disease. She is GBC osteochondropathy.
- Osteochondrosis dissecans. In different sources it can be called Koenig's disease.
- Diabetic osteoarthropathy. Diabetic complication.
- pseudogoutAlso chondrocalcinosis.
- Intermittent hydrarthrosis is an overproduction of synovial fluid.
- Synovial chondromatosis (Lotsch syndrome).
Also, the leg in the area of the hip joint in pregnant women often hurts.
During this period, complex hormonal changes occur, the growing uterus displaces neighboring organs and strains the ligamentous apparatus of the hip joint. Also, weight gain increases the load on the legs. If dietary recommendations are not followed, a pregnant woman may develop a lack of calcium, due to this mineral imbalance, the structure of bones and joints is disturbed.
Causes of pain
The prevalence of arthralgia increases with age.In children, symptoms of TBS disease (hip joint) occur with a frequency of no more than 10%, and in the elderly - 50%. Most women suffer from this pathology. This is due to age-related hormonal changes after menopause.

Why does the hip joint hurt? There is no definitive answer to this question as the list of reasons is quite long.
The main factors causing arthralgia in the hip joint:
- Pathological process within the musculo-ligamentous apparatus. In most cases, this is a consequence of direct mechanical action - a bruise on the joint with subsequent inflammation of its components.
- Anatomical changes in the joint. They can be congenital or post-traumatic (dislocations, fractures).
- Pathology of other systems. Inflammation of the TM (small pelvis) organs can spread to the pelvic bones. Neurological disorders are manifested by pain of any location. Metabolic disorders cause a mineral imbalance. The bone-ligamentous connection is weakened, the risk of injury increases.
Inflammatory and infectious processes in the joints and surrounding tissues.
The most common cause of arthralgia of any location is suppuration of the musculoskeletal joint.
Inflammation in the hip joint is classified into:
- Primary. It is formed with the direct penetration of pathogens into the joint - a blow with a sharp or blunt object with the formation of a wound.
- Secondary. TBS infection occurs from a distant focus of inflammation: by contact or hematogenous route.
Arthritis TBS
It occurs mainly in elderly patients.Aching pain in the hip joint, aggravated by walking, radiates to the groin, perineum and thigh. It is difficult for the patient to get up from a chair or climb stairs without help. Discomfort worse in the morning.
Therapy involves taking anti-inflammatory drugs and introducing glucocorticoids into the intra-articular bursa. If necessary, your cavity is drained.
Rheumatoid arthritis (RA)
This is a chronic systemic connective tissue disease similar to polyarthritis.The essence of this pathological process is inflammation of the synovium, cartilage and joint capsule. The reason is a dysfunction of the immune system. Characterized by polyarthralgia, stiffness of movements in the morning, high fever is possible.
The shoulder and hip joints are very rarely affected, the pain appears only in a late stage of RA after a couple of years from the onset of the disease.
Acute septic arthritis
This is an infectious childhood disease, 70% of cases occur in babies under 4 years of age. The causative agent is usually Staphylococcus aureus. The child refuses to walk due to severe, sharp pain in the hip joint and groin when moving. Characterized by high fever and increased excitability.
Treatment involves removal of the effusion from the joint cavity and antibiotic therapy.
The risk of developing osteomyelitis and sepsis is high.
Tuberculous coxitis or arthritis
Very often, pediatricians are faced with this disease. In young children, the immune system is underdeveloped, which leads to the possibility of infection.
This disease is characterized by slow progression. Initially, the child gets tired very quickly, her activity decreases, she stops running. Gradually, atrophy of the thigh muscles occurs. Movements are hampered. Pain in the hip joint in a child acquires a character of severe pain, the limb becomes longer than a healthy one.
If the pus melts the synovial membrane, the exudate spreads along the muscles and tendons, forming phlegmons and fistulas.
In the absence of complications, conservative treatment is performed.
Tendovaginitis in the hip joint area.
This pathology is an inflammation of the tendon of the muscle and its vagina. Caused by prolonged overuse or leg injury.
The main complaints: the femoral joint hurts when moving, the lesion swells, the change in the gait, the lameness becomes noticeable.
Treatment - medication: anti-inflammatories, intra-articular injections of corticosteroids.
Bursitis
Of all the synovial bursa, the bursa of the acetabulum is the most frequently inflamed.It partially covers the femur. With hip bursitis, the pain radiates to the thigh and gluteal region. The patient can not lie on the affected side - the pressure in the synovial sac increases and the pain intensifies.
If there are no complications with bursitis, treatment consists of unloading the lower extremity with a cane or crutch.
Medications: Analgesics and corticosteroids.
Idiopathic ankylosing spondylitis
This is a chronic inflammation of the spine and elements of the sacroiliac joints.
The disease is dangerous for its complications that reduce the standard of living and lead to disability.
If you find such a problem, you should immediately contact a specialist for the appointment of the correct treatment.
The etiology is not entirely clear. Modern medicine suggests that the main cause is hereditary predisposition. Most of the time, people under the age of 30 get sick.
Symptoms of idiopathic ankylosing spondylitis:
- Increased body temperature, fever.
- Intoxication syndrome: malaise, weakness, lack of appetite, weight loss, sleep disturbances.
- Constant dull pain in the hip joint, as well as at the level of the sacrum and buttocks, extending along the back of the thigh. Generally bilateral, at night its intensity increases.
- Limited mobility in the lower back and hips. This symptom gradually spreads to the overlying sections of the spine along the entire length of the back, including the neck. As a result, the patient takes a forced "petitioner's stance".
Rehabilitation therapy is based on special physiotherapy exercises for joint development.
Medications: NSAIDs to relieve pain and inflammation, corticosteroids.
tendinitis
Athletes or people whose work is associated with heavy physical labor are prone to tendon inflammation. Characteristic of the manifestation: aching pain in the hip joint occurs with a large load on it. At rest, discomfort is usually not observed.
It is recommended to reduce the load on the leg, in advanced cases - bed rest.
Pharmacological treatment: NSAIDs, topical analgesic gels, glucocorticoids, chondroprotectors.
Syphilis
In the late stage of the disease, the bones and joints are affected. Gum formation is characteristic. Its excessive pathological mineralization occurs. TBS is extremely rare.
Gumma - a nodule in the tissues, formed during advanced syphilis, destroying the surrounding tissues. The process ends with the formation of rough scars.
Treatment is ineffective, the risk of developing complications in the form of osteomyelitis is high.
Fungal arthritis of the hip
It occurs as a result of prolonged use of antibiotics and with pathologies of the immune system.
People who are infected with HIV or have AIDS are especially susceptible to fungal arthritis.
Pain in the joint is constantly present, has an aching character.
Fungal lesions of the bones are characterized by a tendency to the formation of fistulas, duration and difficulty of treatment.
Therapy: systemic antifungals.
According to the indications, surgical intervention is performed.
Bone and soft tissue tumors
Oncological diseases of the hip joint can be cancer metastases of a distant organ or arise independently.
- Benign tumors of bone tissue - osteomas.
The foreign formation grows, squeezing nerves and blood vessels. The clinic is similar to piriformis syndrome.
- Malignant bone tumors - osteosarcomas.
The neoplasm rapidly increases in size, becomes necrotic and disintegrates, spreading metastases throughout the body.The pain in the hip joints at night is excruciating, it does not stop even after taking NSAIDs or trying to anesthetize.
- Mesenchymal tumors are made up of soft tissues. Benign ones rarely recur and do not metastasize. Depending on the aggressiveness of the malignant cells, the intensity of the pain is variable.
Degenerative diseases of the joint
coxarthrosis
Hip osteoarthritis is a chronic disease characterized by a change in the integrity of the articular surfaces, due to a violation of metabolic processes. It develops very slowly, over several years. Initially, cartilage tissue is affected, then bone tissue, followed by varus deformity of the joint and limb. It occurs at the age of 40 years.
Symptoms:
- The hip joint hurts only when walking.
- Stiffness of movements in the TBS.
- As the process progresses, a shortening of the length of the limb is observed.
- Weakness and atrophy of muscle mass.
- Limp.
- When walking, a creaking sound is heard.
- With a bilateral injury, a "duck gait" occurs, which is transferred from one leg to another.
Medications: NSAIDs, vasodilators, muscle relaxants, chondroprotectors, injections of hormonal drugs into the joint cavity.
Local effects: ointments, lotions, compresses.
In the last stage of the disease, surgery is ongoing.
osteochondrosis
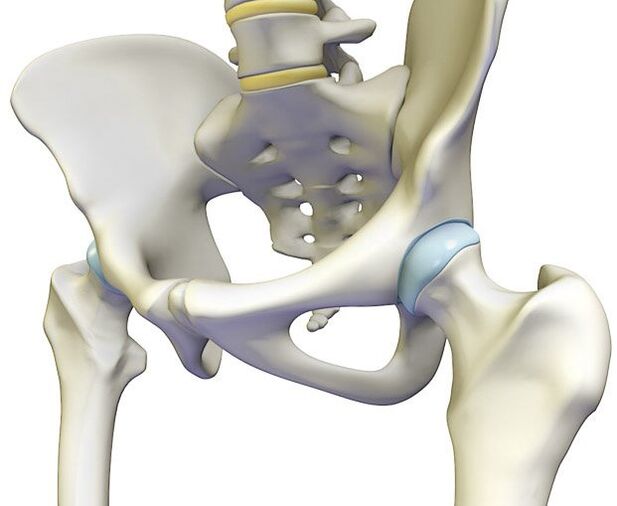
Degenerative changes in the intervertebral discs cause damage to the surrounding tissues.
Symptoms:
- Pain in the lower back that radiates to the hip joint and thigh.
- It's sudden, sharp and sharp. It begins in the lumbar region and buttocks, descends down the back of the leg.
- Unilateral localization of pain is more common.
- The patient takes a forced position, lying on a healthy side.
- Probably decreased sensitivity of the skin of the leg.
Treatment is complex. Anti-inflammatories and analgesics, moderate physical activity (swimming), physiotherapy after remission of the most acute phenomena.
With pronounced pain, it is recommended to do an anesthetic blockade.
injuries
Injury
Pain of moderate intensity is characteristic, during active movements its intensity increases. The first time after an injury to the hip joint, lameness appears, which quickly passes.
At rest, the symptoms disappear.
In order to quickly get rid of pain in case of an injury to the pelvic joint, it is necessary to apply cold to the injury site - an ice pack or a frozen product.
hip dislocation
Perhaps:
- Congenital. It is the result of a failed delivery or pathologies of intrauterine development. The child has uneven gluteal folds and limb shortening, possibly a pinched nerve, manifested by seizures. If the dislocation is not corrected in childhood, the child may later be disabled.
- Traumatic. Signs: intense and sharp pain, complete closure of joint function, massive edema and extensive hematoma appearing over the damaged area. Getting up from a chair or bed becomes impossible for the patient without help.
In case of hip dislocation, you should go immediately to the emergency room or hospital.
fractures
The hip joint is made up of powerful strong bones.
The most common diagnosis in this subgroup is a fracture of the surgical neck of the femur. It is placed mainly on women over 60 years of age.
The cause of such damage is a fall or impact in the area of the TBS.
The strongest pain is felt, the hip joint is pulled and an abscess forms, movement in it is almost impossible. The upper thigh area swells, an extensive hematoma appears. The injured leg is shortened, the patient limps. When moving, a characteristic click is heard.
When a fracture occurs, the surrounding tissues are damaged, which is accompanied by a burning sensation. In the absence of treatment, an inflammatory process can begin here. If the nerve is pinched, you may experience a feeling of numbness in your thigh.
Treatment is complex: surgical and medical.
Specific causes of arthralgia
piriformis syndrome
With the localization of pathological processes in the area of the hip joint, the surrounding tissues are also affected. A long-term spasmodic piriformis muscle compresses the sciatic nerve and its vessels, causing a number of symptoms:
- Leg pain in the region of the hip joint. She goes to the buttocks and the lumbosacral joint.
- Increased discomfort when leaning on the affected leg.
- Piriformis muscle compaction.
- Sudden "lumbago" pain along the nerve.
Etiology: injuries and infectious and inflammatory diseases of the pelvic organs, vertebrogenic pathologies, muscle overtraining, long-term preservation of a non-physiological posture.
Medications: NSAIDs, muscle relaxants, analgesics, blood circulation improvers, glucocorticoids.
After the subsidence of acute phenomena, rehabilitation measures can be prescribed: physiotherapy, massage, acupuncture.
Aseptic necrosis of the femoral head
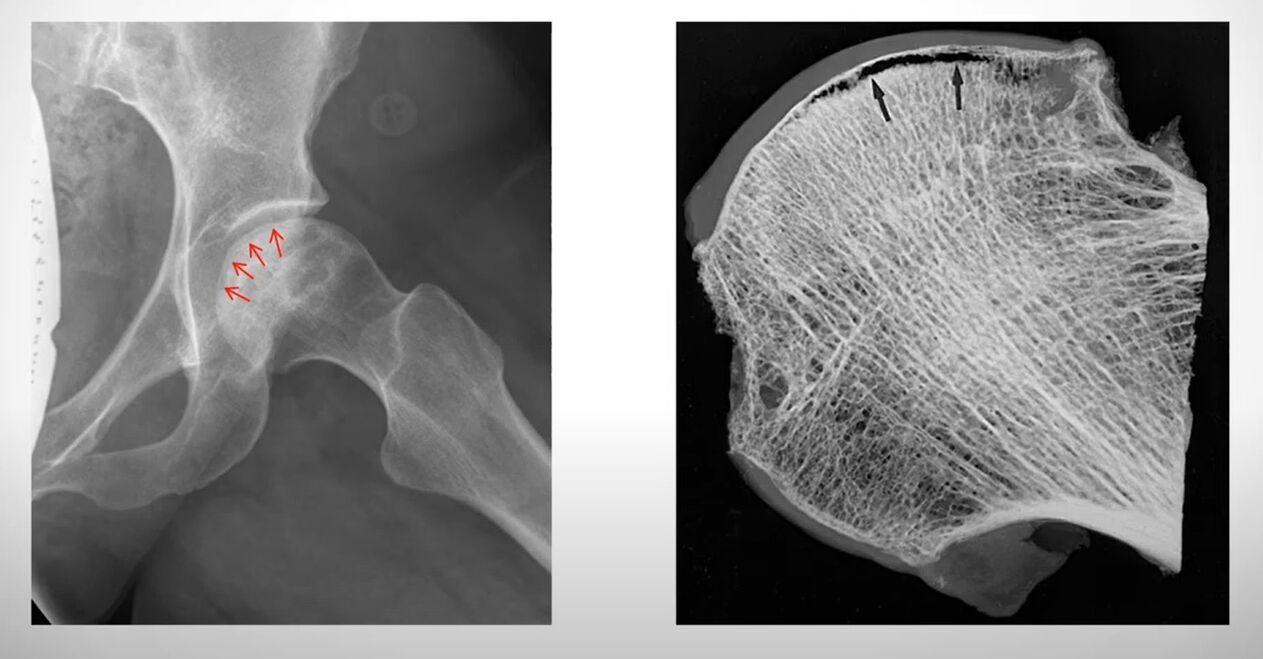
The vast majority occur in young men. The etiology of the disease is ischemia of the upper thigh. With insufficient blood supply to the tissues, their oxygen starvation occurs and their necrosis (necrosis) begins.
Clinical picture: the hip joint hurts and gives way to the leg and perineum. Confidence in the injured leg is not possible. After a few days, the nerve endings melt and the pain goes away. This is a terrible sign! With necrosis of the deeper layers of the bone, the risk of rapid development of osteomyelitis and sepsis is high.
Treatment is surgery and pharmacotherapy.
Koenig's disease
Osteochondritis dissecans - exfoliation of a small necrotic cartilaginous area of the bone and its protrusion into the joint cavity.
This is a rare disease. Typical for men from 15 to 35 years old.
Patients complain of mild pain in the hip joint. The joint "sticks" when moved.
The treatment is conservative (duration 10-18 months) and surgical. During surgical intervention, exfoliated masses are removed, the congruence (comparability) of the articular surfaces is restored.
diabetic osteoarthropathy
Violation of glucose metabolism leads to circulatory disorders and innervation of all organs. Changes in the hip joint are more often unilateral: on the right, it occurs more often than on the left. The immune response is reduced, making it easier for the body to become infected.
Clinical picture:
- Joint swelling.
- The skin that covers it is cold to the touch.
There is no pain syndrome in diabetic osteoarthropathy!
Treatment consists of careful control of blood glucose levels and timely administration of insulin.
pseudogout
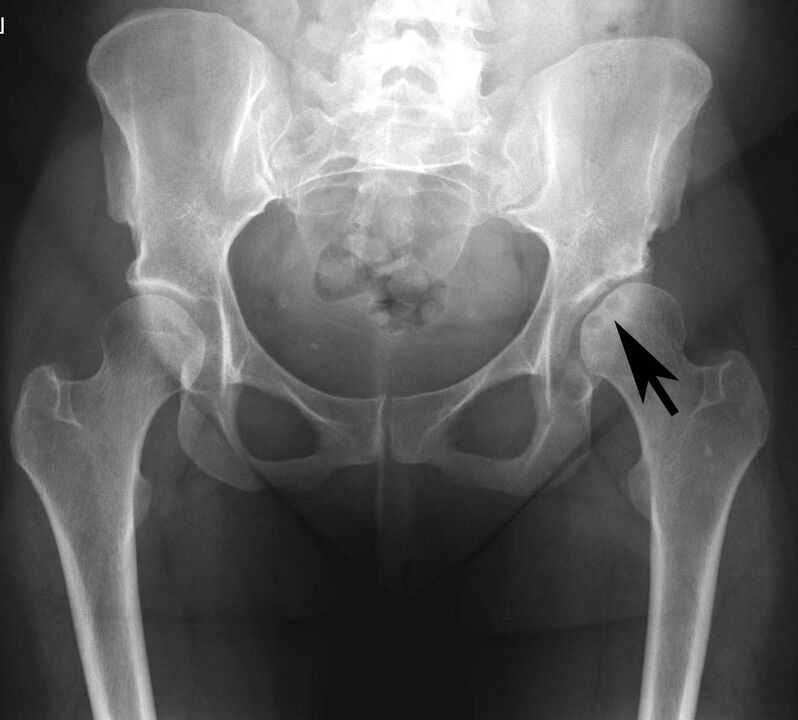
This pathology is the deposition of calcium salts in the articular cartilage.
Doctors associate it with endocrine pathologies: hyperparathyroidism, diabetes, gout, etc.
Symptoms:
- Starting with sharp pain in the hip joint.
Various types of calcium salts are known. With some of them (pyrophosphates), there is no pain.
- Movement in it is limited, abduction of the leg to the side is difficult.
- Edema and hyperemia are characteristic.
- Increased body temperature and fever.
To date, there is no specific treatment. An acute attack is stopped by intra-articular administration of corticosteroids and NSAIDs.
intermittent hydrarthrosis
This is a chronic disease, manifested by episodes of increased production of synovial fluid. prone to frequent relapses.
It is diagnosed mainly in women between the ages of 20 and 40.
The etiology is unknown. There are two theories about the appearance of this disease: associated with injuries and caused by endocrine disorders.
The joint increases in size, becomes stiff.
The attacks pass by themselves in 3-5 days.
Medical treatment is ineffective. Relapses occur even after surgery.
synovial chondromatosis
This benign metaplastic disease is the replacement of synovial collagen by cartilage. The structure of the articular surface changes, as do its properties.
The probability of getting chondromatosis is much higher in men, predominantly middle-aged and older.
The etiology is not clear.
There is local swelling, limited function of the joint, crunches during its work, arthralgia.
The treatment is only surgical.
Hip pain in children and adolescents
epiphysiolysis
This pathology is more typical of children during puberty (from 11 to 16 years). Right now, there is a sharp jump in growth. Due to the weak growth zone, the HBA slips on the neck, causing discomfort in the hip joint.
The child feels pain in the thigh, passing to the groin and knee. Lameness is noted, but confidence in the limb is maintained.
The disorder is surgically corrected. You should start therapy as soon as possible. Otherwise, HBA slippage can lead to the development of arthrosis and joint inflammation.
dysplasia
It is an excessive formation of connective tissue that can replace bone elements. As a result, solid anatomical structures become plastic, flexible. The ligaments, menisci and tendons weaken. An unstable hip is formed, which is distinguished by frequent dislocations.
Dysplasia is an inherited disease that usually occurs in babies between 3 months and 1 year of age. Orthopedists can easily cope with the correction of the fit of the legs.
The latent form can appear in adolescence.
If you notice manifestations of clubfoot or foot deformity in a child, you should quickly go to the hospital for an examination of the baby's musculoskeletal system!
The later dysplasia is detected, the more problematic its treatment is.
osteochondropathy
This group of diseases includes lesions of bone and cartilage tissue, in which the most loaded areas undergo aseptic necrosis.
Etiology: genetic predisposition, hormonal imbalances and infections can cause this pathology.
In 30% of cases, the hip joint is affected. These are predominantly childhood diseases that are common in adolescents during their growth spurt.
At the initial stage, an adult should determine the localization and nature of the pain, contact a pediatrician and obtain the necessary information to prevent the development of complications.
Legg-Calvé-Perthes disease
The syndrome is characterized by HBK necrosis in children under 15 years of age. The right hip joint is the most commonly affected.
The cause of the pathological condition is a violation of blood circulation in the upper leg with the addition of cartilaginous tissue to the process.
Clinical picture:
- Initially, the head of the femur hurts. With the progression of necrosis, arthralgia suddenly disappears. This indicates the death of sensitive organ receptors.
- Change in gait: the child begins to limp.
- Movement in TBS is limited.
- Most of the time unilateral.
Complications: dislocation, coxarthrosis, lower limb deformity, muscle atrophy.
diagnostic measures
Before prescribing treatment, the doctor must carefully study the complaints, anamnesis and conduct an examination.
In case of hip joint disease, the following studies are necessary:
- Laboratory blood tests (with inflammation, ESR is increased, and leukocytosis is observed).
- Simple x-ray of the joint in two or more projections.
- MRI with or without contrast.
- MSCT. It is used to check for the presence of a sarcoma.
- osteoscintigraphy. radionuclide method. The most common and informative type of examination of bone tissue.
- Ultrasound of the hip joint.
- Densitometry. Needed to determine bone density and strength.
If the patient cannot sit or stand, and pain relief is useless, he is immediately sent to the hospital for further surgical treatment.
When to see an emergency doctor
- When there is a sharp pain when moving in the hip joint.
- If it is impossible to support the affected leg.
- Detection of edema of the lumbar and femoral region.
- Redness or bruising in the affected area.
There are popular ways to relieve pain in the pelvic joint. Relying on these tips for a quick cure is not worth it. Without a complete diagnosis, it is impossible to determine the cause of arthralgia, and self-medication will lead to the development of complications.































